Functional Nutrition Testing for Hair Loss: The Root Cause Approach
When Hair Loss Becomes Personal
Hair loss is a common issue we see at 23 Nutrition Therapy. It carries both emotional weight and physiological meaning, and it often appears long before other signs that the body needs support. At our clinic, we use root cause functional medicine to help clients understand what their hair is communicating about their health.
One of our functional nutrition coaches experienced hair loss firsthand. This is her story…
I found myself standing in the shower one day with clumps of hair in my hands, knowing it was far too much to wash down the drain. It was the first time I realized this was more than just hair loss.
My body was signaling that something more profound was happening. Not normal shedding or a few loose strands you find on the glass shower door. Clumps. This is when showering stopped feeling relaxing and started becoming something I had to mentally prepare for.
At work, I would run my fingers through my hair the way I always had, only to feel strands slip out and get caught between my fingers. I would watch them fall to the floor or quickly gather them in my hand and tuck them into my purse before anyone noticed. 
Late at night, I even found myself scrolling through hair extension costs and hormone articles, trying to take back some sense of control and understand how something so foundational to my sense of self could start disappearing.
I couldn’t understand why it was happening at 27, at a time in my life when Is supposed to feel healthy and vibrant.
My experience was not unique. Many people come to our practice feeling the same fear, confusion, or sense that their body is shifting in ways they don’t yet understand.
Hair represents vitality, identity, and femininity for many women. When it begins to thin or fall out, it can feel destabilizing.
Hair loss is a symptom that refuses to stay quiet. It is a daily, visible reminder that something inside the body needs support.
What began as an overwhelming experience eventually became a turning point. Through the same functional nutrition frameworks we use in our practice, I uncovered the deeper contributors behind my hair loss, including thyroid dysfunction, chronic stress, nutrient deficiencies, and mold exposure. Supporting those areas allowed my hair to gradually grow back healthier than ever.
In this blog, we will walk you through the functional nutrition approach to hair loss, the physiology behind it, the lab markers we assess, and the nutrition and lifestyle strategies that help support healthy regrowth from within.
Why Hair Loss Happens: A Combination of Many Factors
Hair loss rarely has a single cause. It is the downstream result of multiple systems under strain. Hormones, thyroid health, nutrient depletion, toxic exposure, inflammation, and stress dysregulation all intersect and influence the hair growth cycle. When one or more of these areas become imbalanced, the hair follicle receives fewer resources and eventually shifts out of its growth phase.
Hair growth requires a lot of energy. When the body senses stress, inflammation, or nutrient scarcity, it redirects that energy toward vital organs like the heart, lungs, and brain. Since hair isn’t required for survival, the body pauses its support the moment resources feel low.

At the cellular level, oxidative stress and mitochondrial dysfunction impair the follicle’s ability to remain in the active growth phase known as anagen. Studies show that proinflammatory cytokines such as TNF-α, IL-6, and IFN-γ can disrupt the stem cell niche that fuels follicle regeneration, leading to a cascade of miniaturization and premature follicle shedding.¹² In simpler terms, inflammation sends signals that interrupt the follicle’s ability to grow strong, healthy hair. When this happens consistently, hair becomes thinner, sheds more quickly, and takes longer to regrow.
Comprehensive functional lab testing reveals these underlying mechanisms, enabling treatment to move beyond symptom management into restoration.
Hormones and Hair Loss
The Thyroid Connection
Thyroid disorders such as Hashimoto’s and hypothyroidism are among the most common endocrine drivers of hair loss. Thyroid hormones, especially triiodothyronine (T3), directly regulate keratin gene expression and dermal papilla cell proliferation.² These are the processes that help hair grow strong, anchored, and healthy. What this means is that T3 acts like the “on switch” for hair growth at the follicle level.
When thyroid hormone production slows, metabolism drops, nutrient absorption declines, and follicles lose the cellular energy needed for regeneration. This means the body has less fuel available to support hair growth, even if your diet is dialed in. Both estrogen and progesterone are also closely tied to thyroid function and influence the strength and elasticity of hair shafts. When these hormones fluctuate, the quality and texture of hair often change with them. Conversely, hyperthyroidism, or excess thyroid hormone, can also promote hair shedding by accelerating the follicle life cycle.
This is why, for those with Hashimoto’s or hypothyroidism, finding the right thyroid medication and dose is foundational. Working closely with an endocrinologist or primary care physician ensures the medication and dosing are appropriate for your physiology. Undermedication or using the wrong formulation can keep hair shedding unresolved. Many clients notice improvement after transitioning from synthetic levothyroxine to desiccated thyroid or a compounded T4/T3 blend that better supports hormone conversion at the cellular level. In simpler terms, people convert thyroid hormones at different rates, so using the form that matches your body’s needs can make a real difference.
Comprehensive testing is key, which is why we encourage full thyroid panels that include Free T4, Free T3, Thyroglobulin Peroxidase (TPO), and Thyroglobulin Antibodies (TgAb), in addition to TSH. These markers enable providers to identify autoimmune activity and guide clinicians in optimizing treatment based on how the body is actually utilizing thyroid hormone.
If the thyroid isn’t balanced, the body struggles to absorb and utilize nutrients efficiently. Even with a well-structured nutrition plan, hair loss may persist until thyroid function is supported.
Other Hormonal Imbalances
Across a woman’s lifecycle, from reproductive years to perimenopause and beyond, hormone fluctuations play a major role in hair health. High androgen levels in conditions such as Polycystic Ovarian Syndrome (PCOS) can cause thinning, increased shedding, and receding along the hairline.
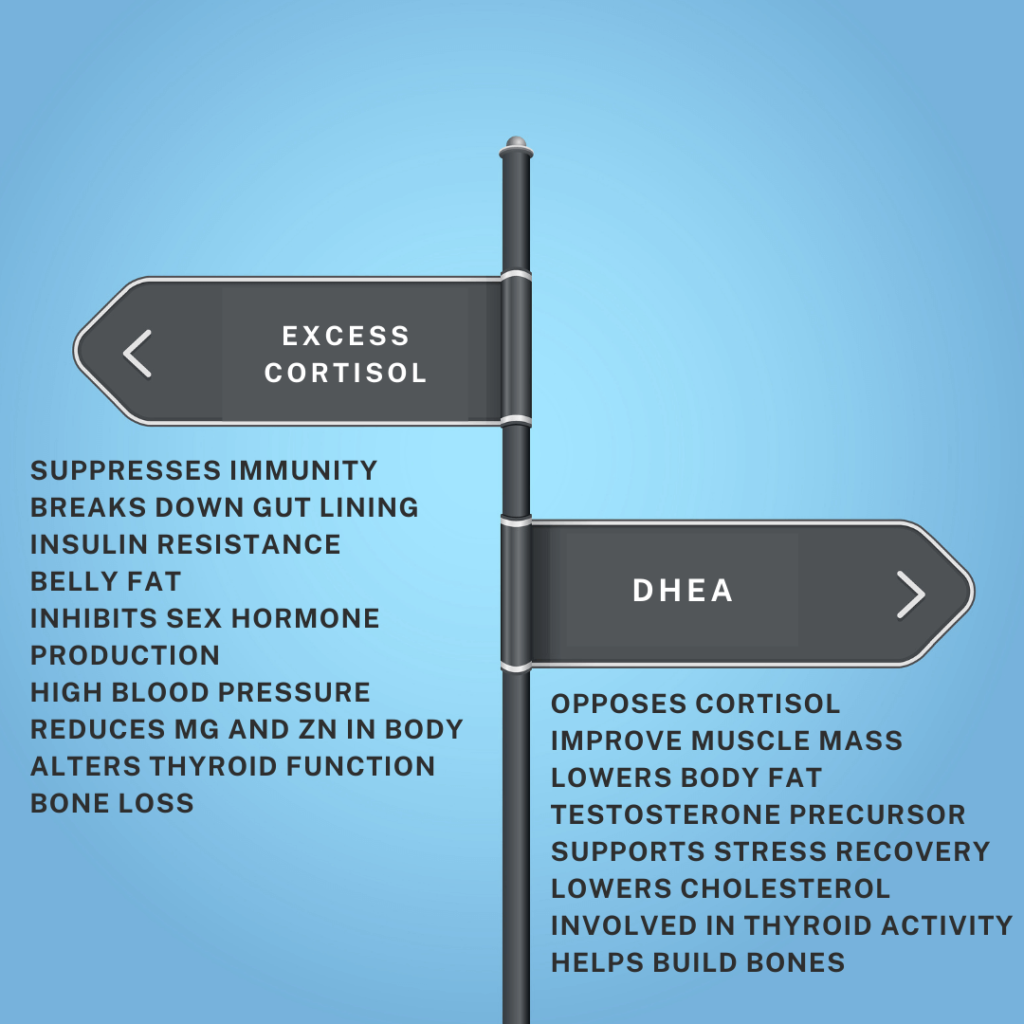
Androgens are a group of hormones that include testosterone and DHEA. They are present in both men and women, but women are more sensitive to changes in these hormones. When androgens rise, they can shrink hair follicles and shorten the growth phase, resulting in visible thinning.
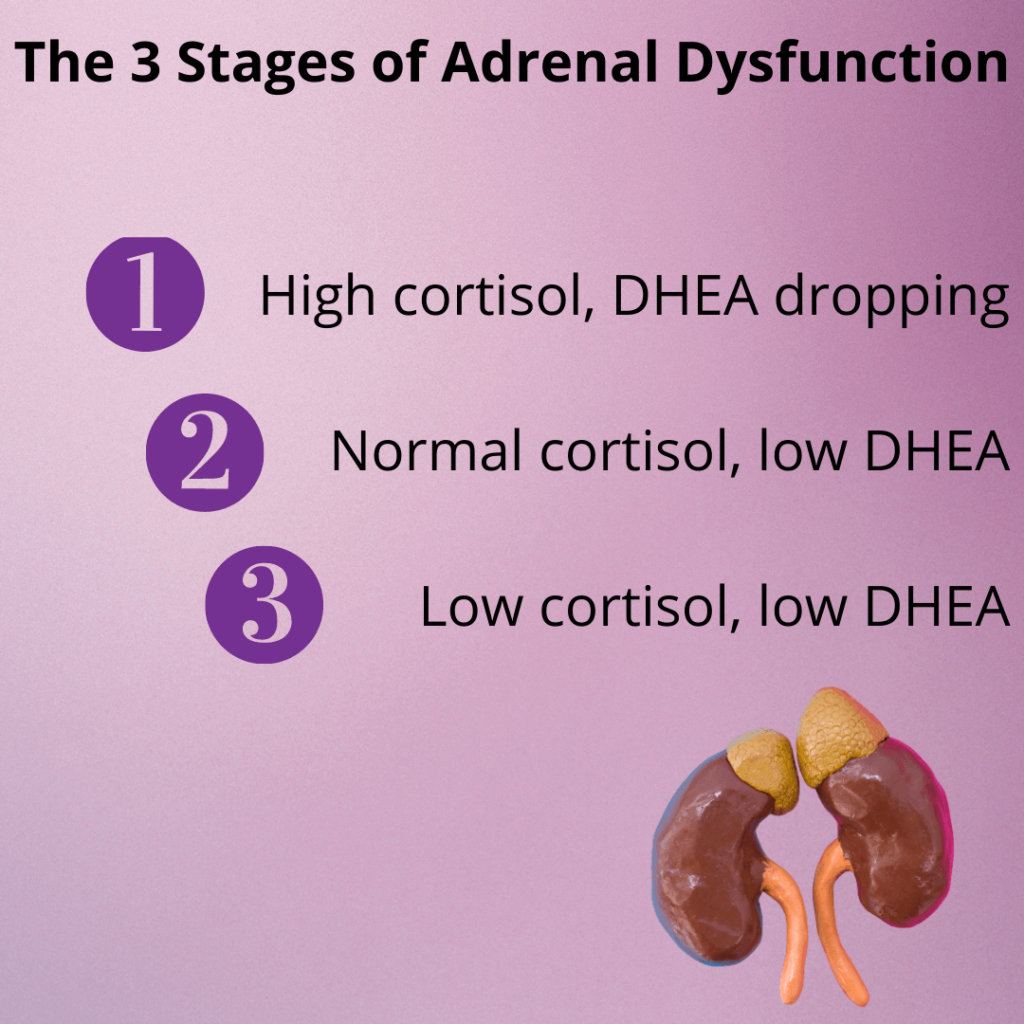
Elevated cortisol levels from chronic stress disrupt the hair cycle by pushing follicles into the resting phase, known as telogen, which is the hallmark of telogen effluvium.¹ In simpler terms, high stress hormones tell the body to pause hair growth so it can conserve energy for survival.
Cortisol also alters follicular cycling and impairs mitochondrial ATP production, which reduces the energy available for hair growth. It can decrease scalp blood flow and weaken collagen around the follicle. This means the hair grows back more slowly and with less strength. Put simply, stress interferes with both the energy and the structural support the hair follicle needs to thrive.
During perimenopause, fluctuating estrogen and progesterone levels can lead to weaker strands and slower regrowth. Estrogen supports fuller, denser hair, while progesterone helps balance androgens. When these hormones shift, hair often becomes thinner, drier, or more fragile.
Balancing hormones through nutrition, stress management, and adequate sleep helps restore communication between the endocrine and integumentary systems, which act as the internal and external mirrors of health. This is why supporting hormonal balance throughout a woman’s life is key to restoring not just healthy hair, but overall vitality.

Minerals and Nutrient Deficiencies
Iron deficiency is one of the most common causes of hair loss, reflecting impaired oxygen transport at the cellular level. Iron supports cytochrome c oxidase activity within mitochondria, which is essential for energy production and follicle growth.⁴ In simpler terms, without enough iron, the follicle does not receive the oxygen and energy it needs to stay in a healthy growth cycle.
Even when ferritin levels appear normal, inflammation can mask deficiency. This is why we encourage clients to complete a full iron panel, including complete blood count, iron saturation, and ferritin together, to offer a more accurate picture in our basic blood panel workup at 23 Nutrition Therapy. Examining these markers together gives a more accurate picture than ferritin alone.
Zinc, selenium, and magnesium are equally crucial for hair health. Zinc regulates DNA transcription and the activity of antioxidant enzymes such as superoxide dismutase. Selenium activates glutathione peroxidase, which helps protect hair follicles from oxidative stress. Magnesium supports keratinocyte differentiation and stabilizes ATP, the molecule that powers cellular growth.⁵,⁷ Simply put, these minerals help hair grow, protect the follicle from damage, and allow the growth phase to continue as it should.
Heavy metals such as mercury, lead, and arsenic can block nutrient utilization and damage hair follicle stem cells. These substances compete with minerals the body needs, making it harder for hair to grow strong and healthy. When heavy metals are present, nutrients are not absorbed effectively, and follicles struggle to regenerate.
This is why expert interpretation of functional nutrition testing, such as the Individualized Optimal Nutrition (ION) test by a functional dietitian, is essential in the clinical context. A functional dietitian can identify nutrient deficiencies, mineral imbalances, and toxic exposures within the larger clinical context, ensuring that hair loss is addressed at the root cause.
How does Mold Exposure and Mycotoxin have anything to do with hair?
When hormones, nutrients, and stress are optimized, but hair loss persists, mold exposure may be an overlooked factor. Mycotoxins, which are toxic compounds produced by mold, can impair thyroid peroxidase and deplete glutathione, increasing oxidative stress and contributing to hormonal imbalance.⁹ In simpler terms, mold toxins place strain on the thyroid and the body’s main detox system, making it harder for hair follicles to grow and repair.
Testing for mycotoxins through urine analysis can uncover a hidden toxic burden that stalls recovery. This type of testing helps identify whether environmental exposure is contributing to persistent hair loss and guides targeted detoxification support.
Nutrition for Hair Health: What to Eat and Why
Hair follicles require a continuous supply of nutrients to synthesize keratin, maintain scalp integrity, and fuel mitochondrial energy. A whole-food diet rich in protein, omega-3 fatty acids, and micronutrients supports this at the cellular level.
- Protein: provides the amino acids cysteine and methionine, which are essential for keratin production and glutathione synthesis. These amino acids strengthen the hair shaft and support detoxification pathways. High-quality sources include grass-fed bison, chicken, and turkey
- Omega-3s: Found in low mercury fish such as salmon and sardines, as well as plant sources like flaxseed. Omega-3s help reduce NF-kB activity, a major inflammatory pathway that affects the scalp, and they improve circulation to the follicle. This means improved blood flow, less inflammation, and more nutrient delivery to the hair root
- Vitamin C: Regenerates iron from its ferric to ferrous form, enhancing absorption, and supports collagen cross-linking around the follicle. Collagen provides structure to the scalp, helping anchor the hair more securely
- Biotin: Acts as a coenzyme in fatty acid metabolism, supporting the lipid layer of hair follicles and overall shaft strength.¹⁰ Biotin helps follicles maintain their protective barrier, which keeps hair resilient
- Leafy greens, nuts, and seeds: Provide magnesium, zinc, and selenium, minerals essential for cell turnover, thyroid function, antioxidant defense, and hormone balance. These minerals help regulate follicle activity and protect the scalp from oxidative stress
All of these nutrients, along with amino acids, fatty acids, and organic acids, can be assessed comprehensively in the Individualized Optimal Nutrition (ION) Test. This testing helps determine whether your hair loss is related to nutrient gaps, metabolic imbalances, or deeper root causes.

The Gut–Skin–Hair Axis
Emerging research highlights the gut–skin–hair axis. Gut dysbiosis, an imbalance of beneficial and harmful bacteria, impairs the absorption of key nutrients, including biotin, zinc, and essential amino acids. These nutrients are required for keratin production and healthy follicle function. In simpler terms, if the gut is not functioning well, the body cannot absorb the nutrients hair needs to grow.
Systemic inflammation driven by intestinal permeability, also known as leaky gut, may further accelerate hair loss.¹¹ When the gut barrier becomes compromised, inflammatory molecules circulate throughout the body and disrupt normal follicle cycling.
Functional Nutrition Testing and Support
Functional nutrition testing removes the guesswork by identifying both deficiencies and blocked pathways. Pairing thyroid panels, hormone mapping, iron dynamics, vitamin A status, vitamin D, minerals, amino acids, fatty acids, organic acids, heavy metals, and mold and mycotoxin exposure provides a multi-dimensional view of the body’s metabolic terrain. This type of testing reveals how well your body is absorbs nutrients, produces energy, detoxifies, and maintains hormonal balance, so we can understand why hair loss is occurring.
How to Get Help
Functional medicine nutrition counseling at 23 Nutrition Therapy focuses on restoration, not restriction. It supports cellular resilience, mitochondrial efficiency, and nutrient transport, enabling the body to rebuild from the inside out.
We specialize in identifying the root cause of hair loss through functional testing, nutrition, and hormone optimization. Our team helps interpret labs, restore nutrient levels, and create personalized plans designed for your body’s unique biochemistry when you can’t get answers elsewhere, or baseline markers look “normal.”
Understand how your body works and what triggers your symptoms! Schedule a free 15-minute nutrition Strategy call.
Your body is not broken. It is protecting you until it feels safe enough to heal. Our role is to help you create that sense of safety so your body can remember what it was designed to do.
Ready for a Shift?
Book a 15-minute discovery call to explore how we can support your healing through nutrition, nervous system regulation, and brain retraining practices.

While this all may seem overwhelming on your own, working with a registered dietitian is the best place to start to find the root of your symptoms! Schedule a free 15-minute nutrition strategy call to discuss the best approach for you! This is the very first step before beginning the initial “Comprehensive Root Cause Analysis” appointment. Working with a skilled Kalish Method Practitioner, detoxification specialist, and functional medicine dietitian is essential in developing an individualized plan for long-lasting success!

References
- Hughes EC, Syed HA, Saleh D. Telogen Effluvium. StatPearls Publishing; 2025.
- van Beek N, et al. Thyroid hormones directly alter human hair follicle functions. J Clin Endocrinol Metab. 2008.
- Ito, M., et al. Mitochondrial function in hair follicle morphogenesis and cycling. Journal of Dermatological Science 2013.
- Arck PC, et al. Stress and the hair follicle: exploring neuroendocrine and immune signaling. Exp Dermatol. 2014.
- Rushton DH. Nutritional factors and hair loss. Clin Exp Dermatol. 2002.
- Ozturk P, et al. Zinc deficiency and hair loss: pathophysiology and treatment perspectives. Dermatol Ther. 2020.
- Dinkova-Kostova AT, et al. Selenium and redox signaling. Antioxid Redox Signal. 2018.
- Vormann J. Magnesium: nutrition and metabolism. Mol Aspects Med. 2003.
- Watts DL. The nutritional relationships of manganese. J Orthomol Med. 1989.
- Karunasena E, et al. Mycotoxins and human health: implications for thyroid function. Environ Toxicol Pharmacol. 2016.
- Patel DP, et al. A review of the use of biotin for hair loss. Skin Appendage Disord. 2017.
- Kang JI, et al. Gut microbiota and hair loss: mechanisms linking gut health and hair follicle cycling. J Dermatol Sci. 2023.
- Higgins CA, et al. Stem cell niches and hair follicle regeneration. Trends Cell Biol. 2020.
Image & Educational Resource References
Mosaic Diagnostics. MycoTOX Profile Report: Mycotoxin Exposure Assessment.
Available at: https://mosaicdx.com/wp-content/uploads/2023/08/MDX_Report_MycoTOX_ENG-2.pdf
Mosaic Diagnostics. MycoTOX Profile: Clinical Interpretation and Biomarker Overview.
Available at: https://mosaicdx.com/wp-content/uploads/2023/08/MDX_Report_MycoTOX_ENG-2.pdf





 The Power of Self-Compassion
The Power of Self-Compassion Why Brain Retraining?
Why Brain Retraining?























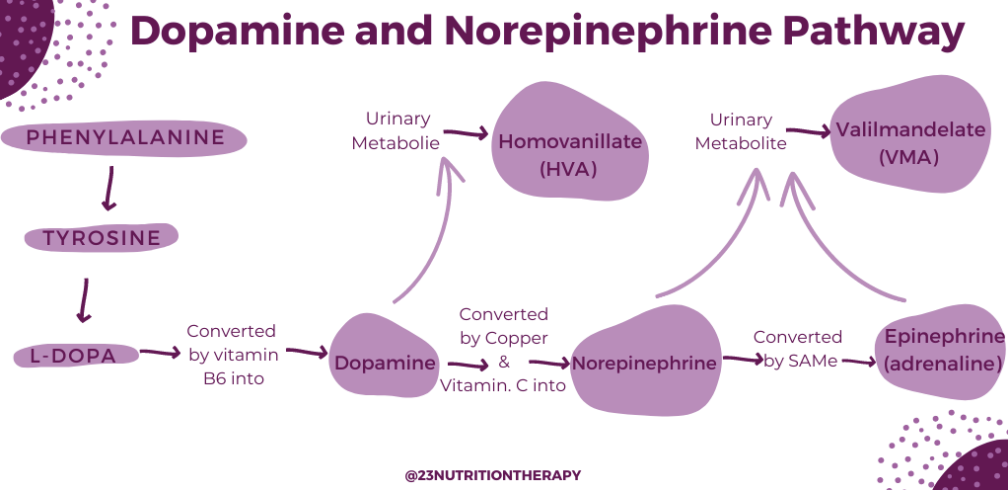 Foods For Neurotransmitters
Foods For Neurotransmitters 
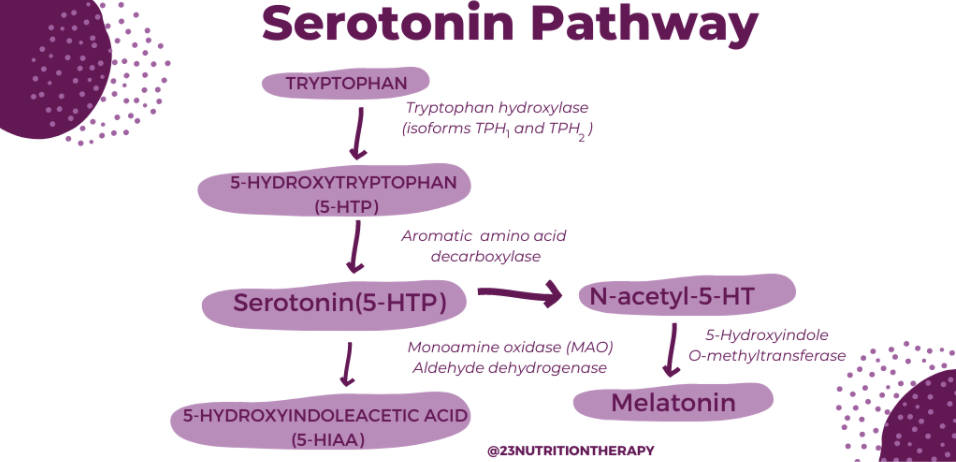 Now that we’ve established the importance of adequate protein intake for balancing our neurotransmitter levels, let’s take a look at the other nutrients and vitamins that are crucial for our brain health.
Now that we’ve established the importance of adequate protein intake for balancing our neurotransmitter levels, let’s take a look at the other nutrients and vitamins that are crucial for our brain health.  Neurotransmitter Testing: Organic Acids or ION
Neurotransmitter Testing: Organic Acids or ION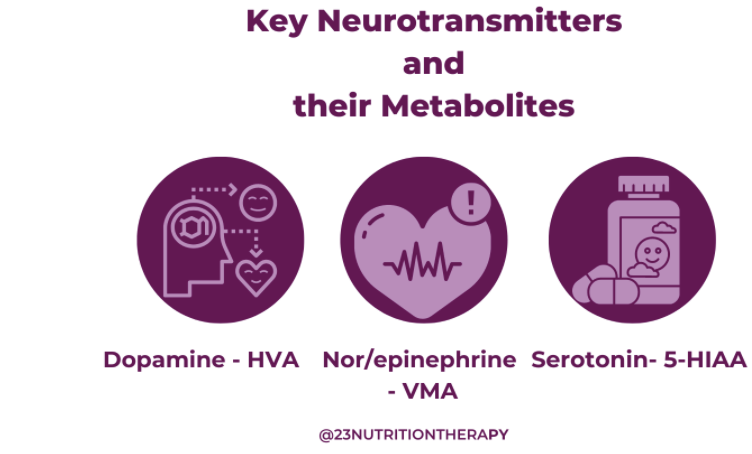
 The Gut-Brain: Gut Hormone Connection
The Gut-Brain: Gut Hormone Connection