Stress is something that, unfortunately, we are all very familiar with. The gut problems that result from stress are also no stranger to most of us.
This blog will explain some of the physiological changes that happen in the body when we’re stressed out that lead to the discomfort you may be feeling.
Can stress cause gastrointestinal problems?
Think of any gut issue, and it’s extremely likely that it is somehow connected to stress. Many of us have experienced an upset stomach from stress at some point in our lives. There are many gastrointestinal (GI) symptoms that illustrate the connection between stress and the digestive system.
Here are some examples of GI symptoms that are related to stress:
- Abdominal pain
- Indigestion
- Heartburn and acid reflux
- Diarrhea
- Constipation
- Nausea and vomiting

To some extent, all of us are familiar with most, if not all, of these uncomfortable symptoms. Here, we will explain why these symptoms occur to explain the connection between stress and the digestive system.
Low Stomach Acid
Contrary to popular belief, the stomach actually produces less stomach acid (concentrated hydrochloric acid – HCl) when we’re under stress. So how does less acid lead to acid reflux and heartburn?
This happens because the sphincter muscle connection between the esophagus and the stomach relies on sufficient stomach acid production to determine when it should be closed. This means, when stomach acid levels are low, the opening stays open and what little acid there is in the stomach can now enter the esophagus and cause heartburn.

Low levels of stomach acid also cause issues with digestion. Certain nutrients may not be as easily absorbed because they won’t get properly broken down without enough stomach acid.
Also, any bacteria we consume with our food (or even bacteria that naturally live in the mouth) may not be killed, which could lead to food poisoning. This can also lead to other dysbiosis (microbial imbalance) issues in the gut, such as SIBO (small intestinal bacterial overgrowth).
Interrupted Bile Flow
Another symptom that is common with stress and the digestive system is interrupted bile flow. Bile is produced by the liver and stored in the gallbladder. When we’re stressed, bile flow is interrupted and grinds to a halt.
Why does this happen? First of all, the stress response suppresses bile release from the liver into the gallbladder because energy is being diverted away from digestive processes and towards your muscles. Also – since digestion stops when you’re stressed, the stomach doesn’t release any food into the small intestine, which is the signal for the gallbladder to pump bile to aid in digestion.
So why is this a problem? The gallbladder is the storage organ for bile, which assists with fat digestion. When the gallbladder is repeatedly inhibited from releasing its bile stores, the entire biliary system gets disrupted.
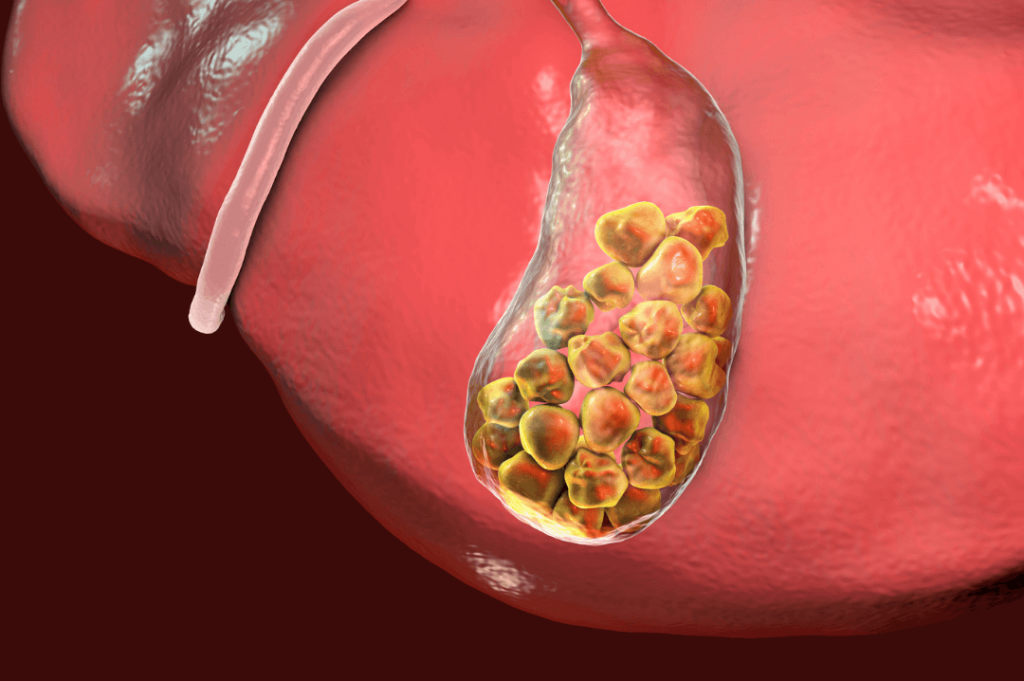
Some issues that can arise include fat malabsorption, fat-soluble vitamin malabsorption, diarrhea, abdominal pain after eating fatty foods, nausea, and feeling heavy after eating. Interrupted bile flow can also cause bile to become over-concentrated with cholesterol and potentially lead to painful gallstones.
Changes to Gut Motility
Gut motility alteration also signals to the connection between stress and the digestive system.
The hormones that are released while you’re stressed out are shown to impact gut motility. This causes the upper gut (your stomach and small intestine) to slow down its digestion process and also decreases the absorption of nutrients. Food stays stagnant in the stomach and small intestine. Stagnant food causes issues such as malnutrition, abdominal distention, bloating, nausea, and vomiting. This is why you can sometimes feel nauseated or even vomit when you’re extremely nervous.
The opposite situation usually happens in the large intestine. During stress, the large intestine speeds up, disregarding its duties of packing our excrement into shape and reabsorbing water. This reduced gut transit time explains why we might experience diarrhea when we’re stressed out.
Heightened Gut Hypersensitivity
Studies also show that sensitivity within the gut increases when we’re under stress. Heartburn and other gastrointestinal (GI) symptoms can actually feel worse when we’re under stress than the same symptoms feel when we’re relaxed.
This relates to irritable bowel syndrome (IBS) – where you experience hypersensitivity in addition to changes in motor function of the gut. Unfortunately, patients with IBS and other GI issues are subject to a vicious cycle where stress contributes to the severity of their symptoms, which then causes even more stress…
Weakened Immune System
Chronic stress can weaken the immune system, making it more likely that we will get sick. When we’re stressed out long-term, the continuous surges of cortisol and other hormones cause widespread inflammation and slow immune cell production, both of which can increase the risk of infection and tissue damage.

Did you know that 60 to 70% of your immune system is in your gut? This makes sense when you really think about it. Our digestive systems are connected to the outside world – humans are essentially just tubes with a lot of complicated accessories.
People consume dangerous pathogens through food and drink every day. Our immune system needs to be especially active in our gut to help protect us from things like food poisoning and small intestine bacterial overgrowth (SIBO).
Hidden Inflammation
Inflammation is valuable in small doses. The inflammatory response is the part of the immune response that promotes tissue healing. Inflammation is supposed to stop once healing is complete, however, this doesn’t always happen. Chronic stress can lead to chronic inflammation, which can then contribute to much larger problems.

Inflammatory bowel diseases (IBD), including Crohn’s disease and ulcerative colitis, are exactly what they sound like – diseases caused by excessive inflammation and irritation in the intestines. These are autoimmune conditions, where your immune system thinks your own cells are foreign enemies. Studies suggest that these diseases are ultimately triggered by disruptions in the immune function within the gut, imbalances in gut microbiota, and leaky gut – all of which can be the result of chronic stress.
A Quick Note About the Gut Microbiome
The bacteria that live in our digestive systems (mostly within the large intestine) are usually beneficial for us. They can produce various products such as essential vitamins and short chain fatty acids that our bodies need.
Each person’s microbiome is as unique as his or her fingerprint. We obtain these bacteria throughout our lives, starting with our journey through the birth canal and continuing with exposure to the environments and foods we are raised with. These bacteria are there to work with the immune system to strengthen the gut lining, prevent inflammation, and protect against any intruding bacteria from colonizing where they don’t belong.
Bacterial Imbalance of the Gut Microbiome
When we experience stress, the gut microbiome is altered. One way this can happen is because when digestion shuts down, any food in the small intestine just hangs out there. This means that our housekeeping system, the migrating motor complex, cannot sweep the small intestine clean of invading bacteria.
Without this housekeeper, any pathogenic or unwanted bacteria that has found its way into our intestines, through our food or from our mouths, is now likely to take refuge there. This can lead to an imbalanced microbiome, uncomfortable GI symptoms, increased colon inflammation, autoimmune diseases like Crohn’s disease, and conditions like SIBO.
Something that you may find really interesting is that your personal microbiome also affects how you respond to stress. Research indicates that people who are able to stay calm during stressful situations have similar microbiomes, which are very different when compared to those who react the most strongly under stress.
The gut-brain connection is bidirectional, but the signals from the gut to the brain are much stronger than the other direction. We know that chronic stress can change both the proportions and the diversity of these bacteria in your gut. So when stress causes an imbalance in your gut bacteria, the newly reigning gut bacteria may actually diminish your resilience to stress.
It all boils down to the gut-brain connection!
When we’re stressed, the nerve that controls digestive functions doesn’t work properly. This contributes to the issues we spoke about above, like low stomach acid, low bile flow, issues with gut motility, inflammation, and more.
This extremely important nerve is called the vagus nerve, and it has become the subject of a lot of research in more recent years. It also has a vast impact on our mental health! The proper function of gut-brain connection via the vagus nerve is essential to maintaining our health and overall wellbeing.

You can get started on some relaxation techniques today in order to improve your vagus nerve function and reduce stress, so that you can achieve optimum gut health and function!
For guided assistance to get to the root cause of your gut problems, schedule your free 15-min appointment today!
I can order your comprehensive stool analysis so we can look for any maldigestion markers, inflammation, dysbiosis, metabolic imbalance, or infection that could be occurring within your gut!
Sources:
http://www.med.unc.edu/ibs/files/2017/10/Stress-and-the-Gut.pdf
https://gut.bmj.com/content/47/6/861
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5859128/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4858318/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1140465/
https://www.sciencedirect.com/science/article/pii/S2352289516300509