There are many approaches to managing and treating IBS and IBS symptoms. The variety of options and the depth of these options may be overwhelming to try and figure out on your own. Let’s dive in!
The Low-FODMAP diet for IBS: What You Need to Know
One common treatment option for IBS is following a low-FODMAP diet. FODMAPs stands for fermentable oligosaccharides, disaccharides, monosaccharides, and polyols, which are types of short-chain sugars (carbohydrates) that are highly osmotic meaning that they draw water into the gut and while they sit and wait, they ferment quickly which can result in poor absorption by the small intestine, excess gas, and watery stool and can cause digestive stress after eating which can result in IBS symptoms being flared.
Switching to a low FODMAP diet is a three step process: elimination, reintroduction, and integration. First, we will eliminate high FODMAP foods from your diet. Then, we will slowly, one by one, reintegrate them into your diet to see which ones specifically cause flare ups of IBS symptoms. Then, once you figure out which ones you can tolerate, you can integrate them back into your diet. Typically, a set of goals will be made along with markers as to how they will be measured. Goals can include things like reducing bloating after meals, decreasing diarrhea/constipation, and/or reducing general abdominal pain.
Along with help from a dietitian, there are many resources to assist with FODMAP identification as well. Some examples of foods high in FODMAPs include wheat, barley, rye, onions & garlic, dates, beans, lentils, hummus, cashews, honey, high fructose corn syrup, milk & yogurt, sugar alcohols (such as those in many sugar-free products), peaches, figs, watermelon, and more.
While eating a whole-food, plant-based diet may help with IBS, it can become tricky to avoid FODMAPs with an already restricted diet. Eating whole foods and certain plant-based products such as tofu and other fiber-rich foods that are gut healthy can improve IBS symptoms however, there is not much concrete research to show that a plant-based or vegan diet will necessarily help with IBS as many plant-based foods are high in FODMAPs and/or are triggering to IBS symptoms due to being ultra highly processed and containing preservatives and additives.
If you are someone who has IBS and wants to eat a plant-based diet, it is highly advisable to work with a dietitian to create a diet plan that meets your desires while also avoiding trigger foods.
 Integrative Therapeutics Physicians Elemental Diet
Integrative Therapeutics Physicians Elemental Diet
The Physicians’ Elemental Diet is a great option for those suffering from a flare up of IBS and IBS symptoms. The Physicians’ Elemental Diet comes in both a regular and dextrose free version and are powdered formulas of medical foods. They are intended for those with diminished gastrointestinal function and are formulated in a way to be easily digested.
The dextrose free formula is the only one we recommend as the risk for fungal overgrowth is increased with dextrose. The dextrose free formula contains higher proportions of protein, lower fat, and lower carb than the standard version.This is a great choice for a 5 day reset to get out of an IBS flare however you must refer to your dietitian to get appropriate amounts of the formula to meet your nutritional needs as this diet is intended to be done under supervision.
Eating out with IBS
It may seem daunting to eat out with IBS, especially given the importance of knowing both what to eat and how to eat so as not to further trigger IBS symptoms. Knowledge and having a plan is key. Working with a dietitian to create a well rounded nutrition plan that supports gut healing is the first step in understanding what foods your body will support and what will trigger IBS symptoms for you.
Once you have this baseline, it will be a lot easier to go out and be able to look at a menu and know what foods your body can and cannot tolerate. With this in mind, it is also important to note the importance of choosing where to eat out and where not to. Going to fast food restaurants with over processed foods that will all trigger IBS symptoms would not be as good a choice as a healthier option would be.
Supplements for IBS Treatment
There are many different supplements that may help treat IBS and IBS-related symptoms. A majority of these will be recommended based on test results from the aforementioned tests such as adrenal support supplements for example.
Other supplements that have been shown to help are herbal antimicrobials for SIBO and other infections, stool binders, biofilm disruptors, gut lining support supplements, pre and probiotics, fiber, digestive enzymes, short chain fatty acids, immunoglobulins, detox support supplements, and nutrient replenishing supplements.
While this might seem overwhelming at first, working with a functional medicine dietitian to narrow down exactly what you need and why is crucial in finding the right treatment plan for you.
Lifestyle Approaches for IBS
Along with nutritional approaches to address the root cause of IBS symptoms, there are a variety of lifestyle approaches that may help in combination with nutritional approaches. As we know, mental health is closely tied into gut health and IBS through the gut-brain axis.
Practicing mindfulness and mindful breathing techniques have both shown to improve mental health and subsequently help improve IBS symptoms. The Nerva app is another alternative option specifically designed to tackle the mental health component of IBS. The Dynamic Neural Retraining System or DNRS, is another mental health approach for IBS symptom management. DNRS helps change the brain’s response to chronic pain/stress stimuli such as IBS symptoms subsequently improving the body’s pain response.
 Other ways of incorporating mindfulness into day to day life is through mindful eating and meal spacing. Making sure to chew food slowly is critical in mindful eating practices. Meal spacing however, allows for the migrating motor complex to go into a state known as rest and digest. The state of “rest and digest” allows the parasympathetic nervous system to function and help the body regulate digestion in a calm state vs in a fight or flight state, the sympathetic nervous system takes charge and that can result in a flare up of IBS symptoms. By spacing out meals, you allow your body to reduce its cortisol levels and induce a state of “rest and digest”.
Other ways of incorporating mindfulness into day to day life is through mindful eating and meal spacing. Making sure to chew food slowly is critical in mindful eating practices. Meal spacing however, allows for the migrating motor complex to go into a state known as rest and digest. The state of “rest and digest” allows the parasympathetic nervous system to function and help the body regulate digestion in a calm state vs in a fight or flight state, the sympathetic nervous system takes charge and that can result in a flare up of IBS symptoms. By spacing out meals, you allow your body to reduce its cortisol levels and induce a state of “rest and digest”.
Another important thing that plays a huge factor in not just our overall health but specifically our gut health is sleep! Getting good amounts of quality sleep is crucial in reducing IBS symptom flare ups. Poor sleep, especially chronic poor sleep habits, can result in an increase in cortisol levels, our bodies natural stress hormone, and can activate the HPA axis which is our bodies natural mediator of stress response. Lack of sleep can cause the gut microbiome to shift resulting in difficulty digesting food and thus a flare up of IBS symptoms. Making sure to get enough good quality sleep each night is crucial in keeping IBS symptoms at bay and reducing intestinal flare ups.

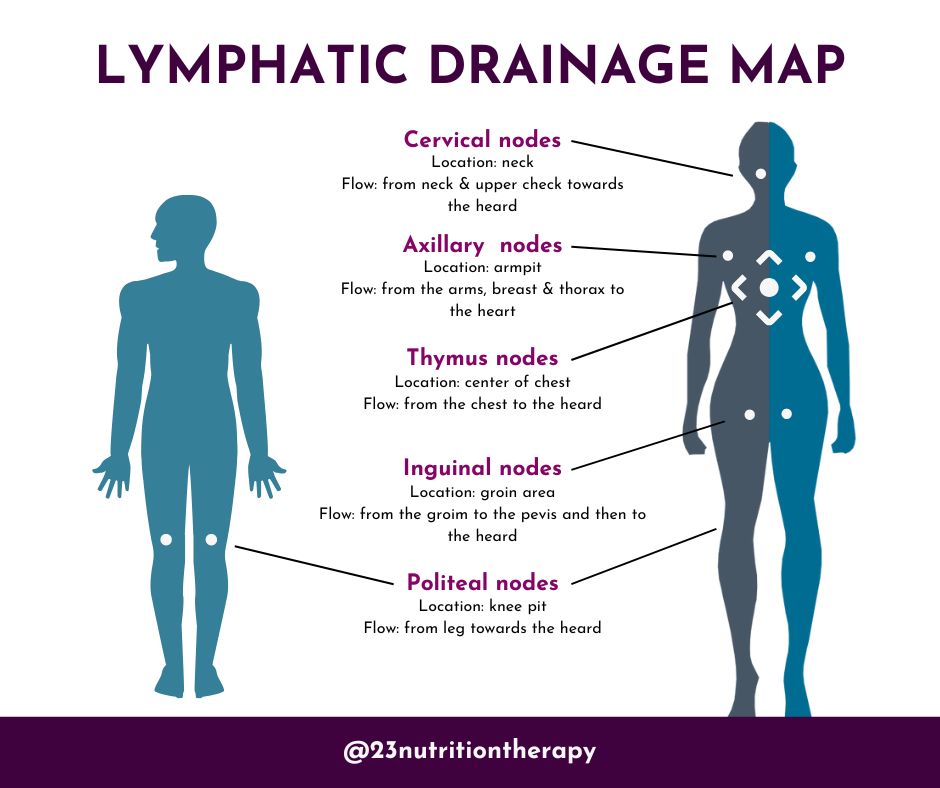
Physical lifestyle approaches have also shown promise in improving IBS symptoms. Osteopathic manipulative treatment (OTM) also known as visceral manipulation, involves physical hands-on manipulation to increase lymphatic flow and restore homeostasis. Another physical approach is vagus nerve toning. A few practices that boost vagal nerve tone include breathing techniques, exercise, mindfulness, meditation, cold exposure, electrical stimulation, and other relaxation techniques.
Another physical approach used in IBS symptom management is through transcutaneous electrical nerve stimulation also known as TENS. A TENS device delivers electrical stimulation that can inhibit pain signals/pathways for specific sites on the body through electrical pulses. Specifically, transcutaneous vagal nerve stimulation, tVNS, which utilizes a TENS device on the left ear, stimulates the vagus nerve system to reduce systemic inflammation. vTNS has been studied for both mental health and gut health, which as we know can go hand in hand, and have shown very promising results without the use of supplementation.
Finding Your System
As we can see, there are a lot of potential approaches to managing IBS symptoms. Each individual will have a different combination of treatments and/or approaches that will work for them. While the abundance of options may seem overwhelming, working with a functional medicine dietitian is key in figuring out the best plan to find the root cause of your symptoms! Are you ready to make a change? Schedule a free nutrition strategy call and get started today.














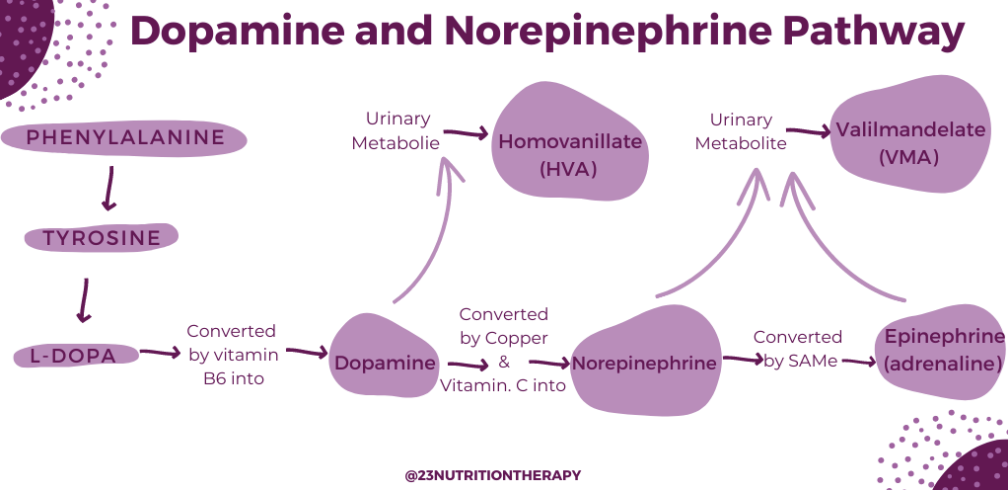 Foods For Neurotransmitters
Foods For Neurotransmitters 
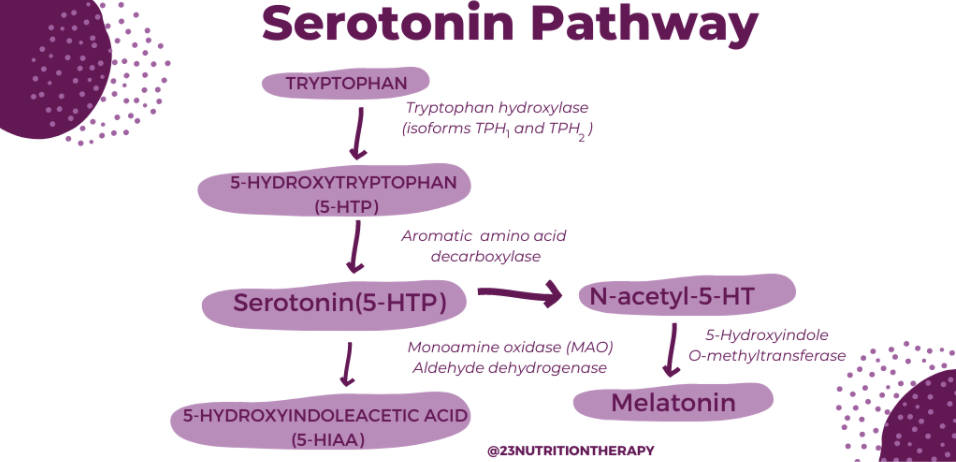 Now that we’ve established the importance of adequate protein intake for balancing our neurotransmitter levels, let’s take a look at the other nutrients and vitamins that are crucial for our brain health.
Now that we’ve established the importance of adequate protein intake for balancing our neurotransmitter levels, let’s take a look at the other nutrients and vitamins that are crucial for our brain health.  Neurotransmitter Testing: Organic Acids or ION
Neurotransmitter Testing: Organic Acids or ION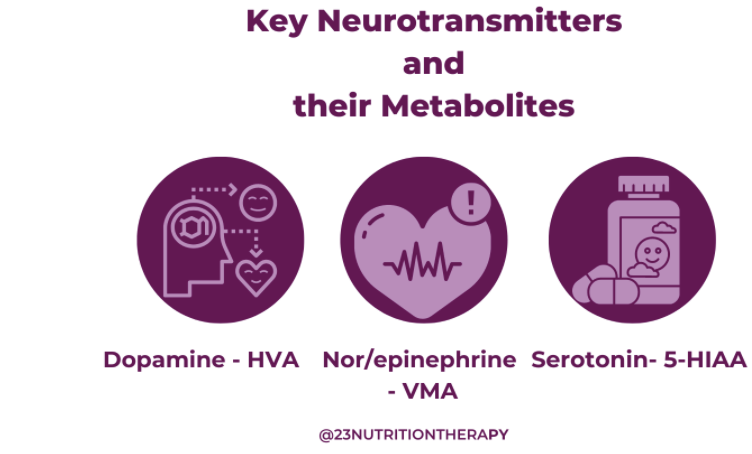
 The Gut-Brain: Gut Hormone Connection
The Gut-Brain: Gut Hormone Connection 
 Increased intestinal permeability becomes an issue when this barrier is compromised and unable to identify or properly separate unwanted substances from the essential nutrients the body needs. When you have a leaky gut, a partially digested protein, allergen, or pathogen can enter the bloodstream. The body will then elicit a natural response better known as inflammation, which in turn causes a further breakdown of the GI tract and a list of symptoms to follow.
Increased intestinal permeability becomes an issue when this barrier is compromised and unable to identify or properly separate unwanted substances from the essential nutrients the body needs. When you have a leaky gut, a partially digested protein, allergen, or pathogen can enter the bloodstream. The body will then elicit a natural response better known as inflammation, which in turn causes a further breakdown of the GI tract and a list of symptoms to follow. 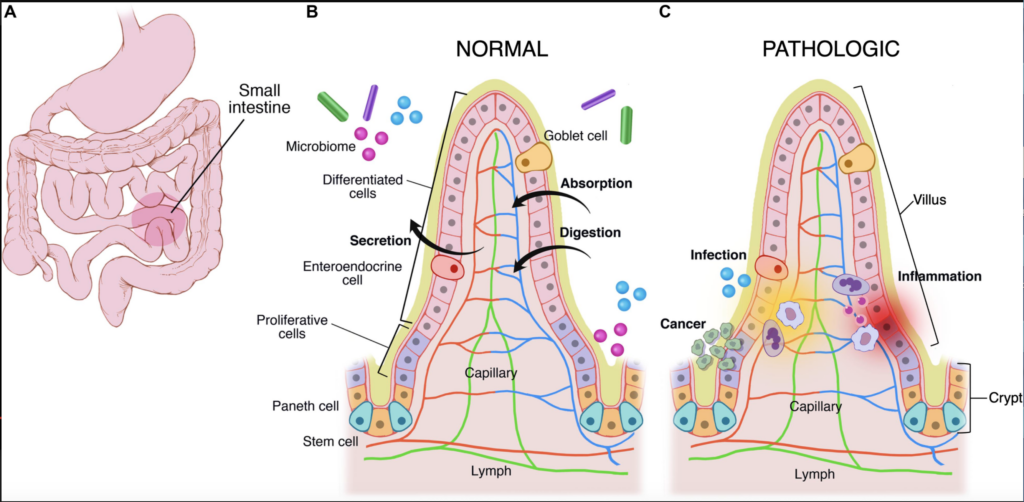 Leaky gut happens when inflammation breaks down the gut lining tissue to make sugar for the blood stream, essentially shredding the gut lining. Now, rather than acting as a selective barrier, the lining becomes more like a sieve. During this process the villi in the intestine become damaged and are now unable to properly absorb fat soluble nutrients. Essential fatty acids, vitamin D, vitamin E, vitamin A, and vitamin K are the main fat-soluble nutrients. They all play integral roles in a multitude of processes in the body. As villi are being destroyed, crypts within the gut lining deepen, hiding parasites and making them difficult to find and treat.
Leaky gut happens when inflammation breaks down the gut lining tissue to make sugar for the blood stream, essentially shredding the gut lining. Now, rather than acting as a selective barrier, the lining becomes more like a sieve. During this process the villi in the intestine become damaged and are now unable to properly absorb fat soluble nutrients. Essential fatty acids, vitamin D, vitamin E, vitamin A, and vitamin K are the main fat-soluble nutrients. They all play integral roles in a multitude of processes in the body. As villi are being destroyed, crypts within the gut lining deepen, hiding parasites and making them difficult to find and treat.  If you suspect you may have leaky gut, consider a stool test to identify any pathogen invasions. After a pathogen killing program, you can begin the healing process by adding more gut-friendly foods to your diet.
If you suspect you may have leaky gut, consider a stool test to identify any pathogen invasions. After a pathogen killing program, you can begin the healing process by adding more gut-friendly foods to your diet. 




 Here are my top tips about optimizing your sleep:
Here are my top tips about optimizing your sleep:

 So, let’s assume that you already have a meal plan and feel that you’re on the road to a completely new lifestyle and better health. (If you aren’t sure where to begin diet-wise, I can help you with your nutrition! Check out what you need to know about becoming a client
So, let’s assume that you already have a meal plan and feel that you’re on the road to a completely new lifestyle and better health. (If you aren’t sure where to begin diet-wise, I can help you with your nutrition! Check out what you need to know about becoming a client  Staying organized with supplements
Staying organized with supplements  Here are some great ways to stick to your recommended supplement protocol:
Here are some great ways to stick to your recommended supplement protocol: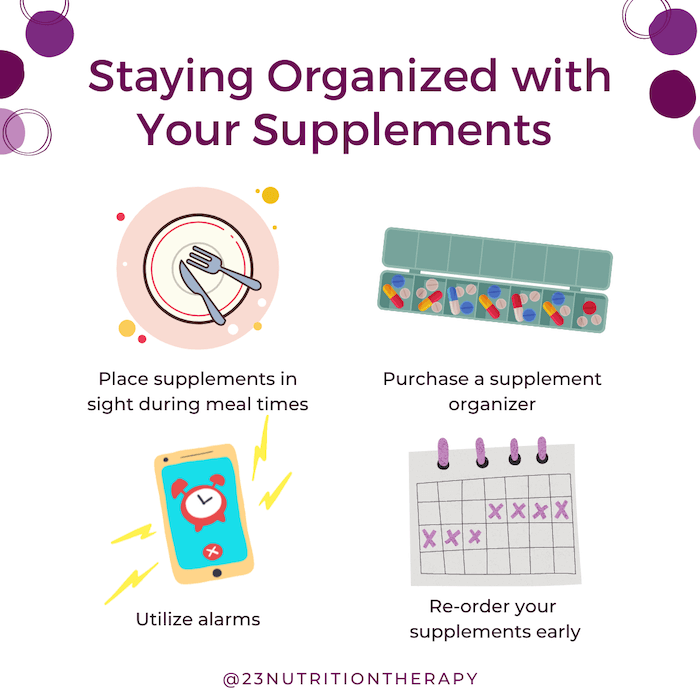
 In the broad sense, food sensitivity refers to the body’s adverse reaction to specific food or chemical antigens (also known as a toxin or foreign substances) causing negative physiological effects within the body. The term “food sensitivity” specifically refers to a delayed, dose-dependent, adverse reaction to food.
In the broad sense, food sensitivity refers to the body’s adverse reaction to specific food or chemical antigens (also known as a toxin or foreign substances) causing negative physiological effects within the body. The term “food sensitivity” specifically refers to a delayed, dose-dependent, adverse reaction to food.